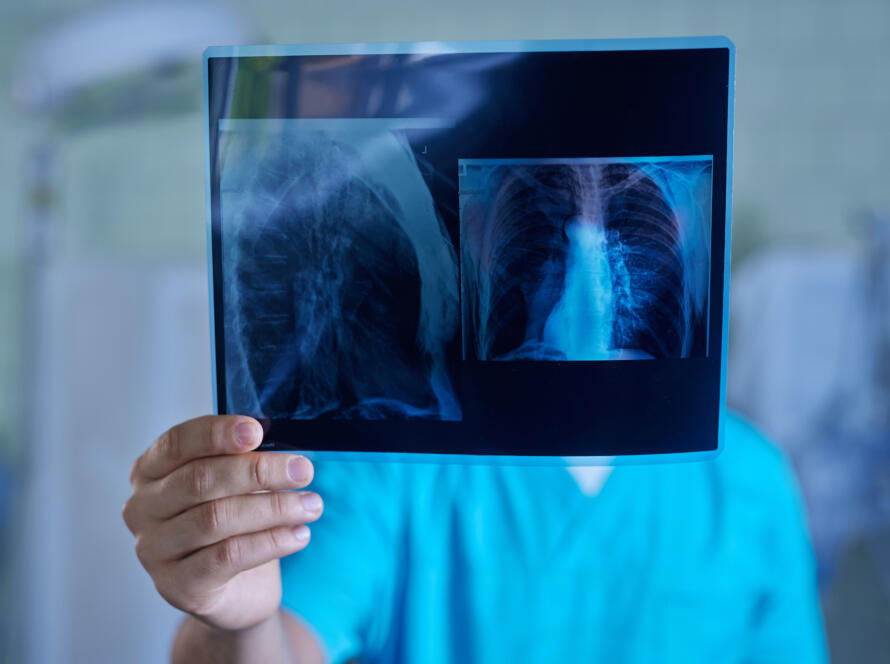
The windpipe (trachea) is our vital primary airway that carries air to the lungs. However, narrowing can sometimes occur in this passage due to various reasons. Our patients often describe this condition by saying, “I have noisy breathing,” “I’m wheezing,” “There is something in my throat, I can’t breathe,” or “I get short of breath immediately while walking.”
Tracheal stenosis (narrowing of the windpipe) can often be misdiagnosed as diseases like asthma or COPD. However, when correctly diagnosed, tracheal surgery can completely open the patient's airway and dramatically improve their quality of life.
Why Does the Windpipe Narrow?
The most common cause of tracheal stenosis is a history of prolonged intensive care and intubation. In patients who have been on a ventilator, the pressure exerted by the tube placed in the windpipe or a tracheostomy cannula can lead to excessive growth of healing tissue (granulation) and impaired blood supply to the cartilage, resulting in a permanent narrowing of the tracheal diameter.
The most common cause of tracheal stenosis is a history of prolonged intensive care and intubation. In patients who have been on a ventilator, the pressure exerted by the tube placed in the windpipe or a tracheostomy cannula can lead to excessive growth of healing tissue (granulation) and impaired blood supply to the cartilage, resulting in a permanent narrowing of the tracheal diameter.
Other causes include:
- Neck and chest traumas,
- Benign or malignant tumors of the windpipe,
- Inhalation burns,
- And sometimes idiopathic (unknown cause) stenosis.
What are the Symptoms? When Should You Suspect It?
If you have recently stayed in intensive care or were intubated, and you are experiencing these symptoms even though your lung health is known to be good, you should definitely consult a Thoracic Surgery specialist:
- Stridor (Noisy breathing): A whistling or wheezing sound that can be heard from the outside while breathing.
- Exertional Dyspnea: Feeling comfortable while sitting but feeling choked when walking or climbing stairs.
- Persistent Cough: A dry cough that does not respond to medication.
Treatment Methods: Dilation or Surgery?
At the Marmara University Faculty of Medicine Thoracic Surgery clinic, our approach to tracheal stenosis patients is determined by the location, length, and structure of the narrowing.
- Endoscopic Methods (Temporary Solutions): This involves opening the narrowing through rigid bronchoscopy (a long metal tube) by passing through with increasingly larger bronchoscopes (dilation), using different bougie dilators, or employing argon laser. These methods provide immediate relief, but the stenosis often tends to recur. In some patients, a stent application may be required to keep the windpipe open.
- Tracheal Resection and End-to-End Anastomosis (Permanent Solution): If the narrowing is in a short segment and the patient's general condition is suitable, the gold standard treatment is surgery. In this operation, the narrowed, diseased part of the windpipe is completely removed. The remaining healthy ends are sewn together (end-to-end anastomosis), restoring the airway to its original width.
Frequently Asked Questions – FAQ
Question: Is tracheal surgery risky?
Cevap: Nefes borusu cerrahisi, hayati bir organ üzerinde çalışıldığı için yüksek deneyim gerektirir. Ancak tecrübeli ellerde (yüksek volümlü merkezlerde) yapıldığında başarı oranı %90-95’in üzerindedir.
Question: Will my voice be hoarse after surgery?
Answer: The vocal cords are located right at the entrance of the windpipe, and the nerves that move the vocal cords are adjacent to the surgical field. Utmost care is taken to protect these nerves during surgery. Although temporary hoarseness may occur, the risk of permanent damage is lower.
Question: Can I move my neck after the operation?
Answer: To prevent tension on the sutures after surgery, we apply a special stitch (Guardian stitch / chin-to-chest stitch) that keeps the patient's chin close to their chest. This stitch is removed after 5-7 days, and the patient gradually begins neck movements.
*This content was produced by Dr. Eyüp Halit Yardımcı for patient information purposes and does not serve academic objectives.