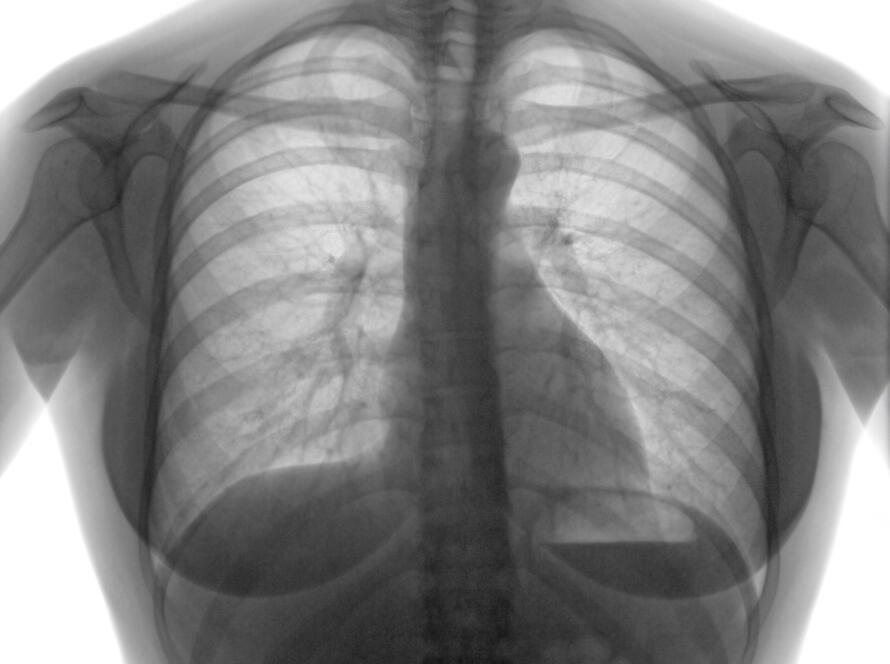
A successful lung or chest wall surgery is only half of the journey. The other half is the recovery period you will spend in the hospital and at home after the operation. While we, as the surgical team, fulfill our responsibilities, you, as the patient, must follow these recommendations to contribute to your recovery.
Our patients' most common concerns involve topics such as drains, pain sensations, and shortness of breath. These are, in fact, natural parts of the healing process. The fundamental rules you should know after surgery are as follows:
1. What is a Chest Tube (Drain)? Why is it inserted?
When you wake up from surgery, you may see a tube in your chest area connected to a drain bottle (or canister). Do not let this alarm you.
- Its Role: Its purpose is to discharge accumulated blood, fluid, and air after lung surgeries, thereby ensuring the lung can expand to its full capacity.
- Precautions: The drain bottle must always be kept below waist level. While walking, going to the bathroom, or lying down, you must be careful not to let the bottle tip over or rise above your chest level.
- When is it removed?: Once your lung is fully expanded on the X-ray and the fluid/air drainage has ceased, your physician will remove the drain, usually with a simple and painless maneuver.
2. Pain: It is not always a bad sign!
There is a common misconception that "if I have pain, something is going wrong." In thoracic surgery, pain is an indicator of tissue healing and active nerve function.
- Pain Management: Do not hesitate to use your painkillers regularly after surgery. For us, the ideal patient is not the "pain-resistant" one, but the "patient who can breathe easily because they are not in pain."
- If you avoid coughing or taking deep breaths due to pain, phlegm will accumulate in your lungs, which can lead to pneumonia.
- Even after you are discharged home, you should continue to take your prescribed painkillers exactly as directed, even if you do not feel immediate pain.
3. Respiratory Physiotherapy: "Lift the Balls"
Your most important "homework" after surgery is respiratory exercises. The Triflo (3-ball incentive spirometer) we provide is a vital tool for opening up your lungs.
How to use it: Place the mouthpiece in your mouth and take a deep breath in to lift the balls and hold them there.
Coughing is Good: Coughing during exercises helps expel internal phlegm and prevents the lung from collapsing (atelectasis). Do not fear that your stitches will "burst"; coughing will not harm your sutures. You can cough safely by supporting your chest with a pillow or your hands.
Inflating firm balloons is also an excellent respiratory exercise.
4. Early Mobilization (Walking) and Nutrition
Lying down doesn't heal; walking does!
- Walk Immediately: Depending on the scale of the surgery, we usually have you up and walking on the evening of the operation or the following morning. Walking prevents blood clots in the legs (embolism) and ensures your bowels are functioning.
- Strong Nutrition: Your body needs protein for tissue repair. You should maintain a protein-rich diet including meat, eggs, and yogurt, and drink plenty of water. Avoiding gas-producing foods reduces pressure on the diaphragm, allowing for easier breathing.
Frequently Asked Questions – FAQ
Question: When will my stitches be removed?
Answer: Nowadays, we use aesthetic and absorbable sutures in most surgeries, so no removal is necessary. If metal staples or non-absorbable sutures were used, they are removed during your follow-up clinic visit 10–15 days after discharge.
Question: Can I take a bath?
Answer: After your drains are removed and your incision sites have dried (usually 2-3 days after discharge), you can take a shower while standing. Avoid scrubbing the wound areas and do not pick at the scabs over your wound.
*This content was produced by Dr. Eyüp Halit Yardımcı for patient information purposes and does not serve academic objectives.